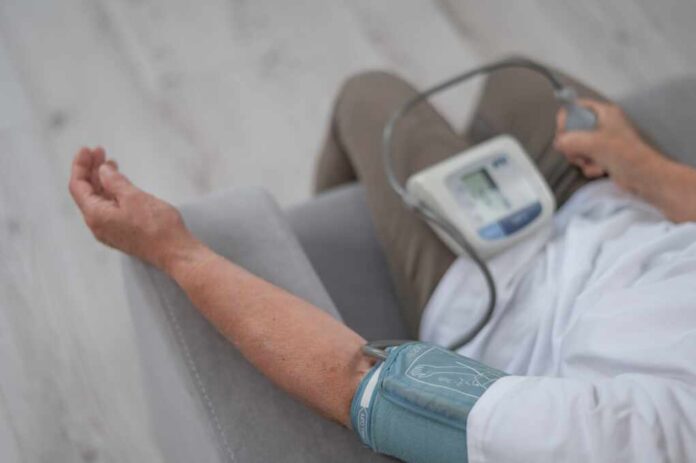
Daily multivitamins show no overall benefit for blood pressure but offer small gains for certain older Americans with poor diets, challenging supplement hype in an era of rising health costs under past administrations.
Story Highlights
- Multivitamins failed to reduce hypertension or blood pressure across the entire COSMOS trial population of older adults.
- Small, statistically significant benefits appeared in subgroups with poorer diet quality and normal baseline blood pressure.
- Researchers emphasize nutrition as the foundation for blood pressure control, positioning multivitamins as a potential adjunct only for the nutritionally deficient.
- Experts warn against overgeneralizing results, stressing “food first” over supplements for most people.
COSMOS Trial Reveals Targeted Effects
Mass General Brigham researchers analyzed data from the COSMOS trial, a large randomized, double-blind, placebo-controlled study of older adults. The trial followed men aged 60 and older and women 65 and older for a median of 3.4 years. Participants received daily multivitamin-multimineral supplements or placebo. Overall, 1034 incident hypertension cases occurred in the supplement group versus 1039 in placebo, with a hazard ratio of 0.98 and no significant difference in blood pressure changes.
Daily multivitamins quietly lower blood pressure in some older adults https://t.co/bIbm4UPakA
— #TheRebelDemocrat (@ejnyamogo) December 14, 2025
Subgroup Benefits Emerge for Poor Diets
Among participants with lower diet quality, measured by Alternative Healthy Eating Index and Alternate Mediterranean Diet scores, multivitamin use is linked to reduced hypertension risk compared to placebo. Those with normal blood pressure at baseline saw small but statistically significant blood pressure reductions over about two years. Lead author Rikuta Hamaya, MD, PhD, MS, noted multivitamins might help those with poorer nutritional intake, though effects remain exploratory and modest.
These findings contrast prior small trials suggesting broader benefits. Micronutrients like magnesium, potassium, and B vitamins may regulate blood pressure, particularly when diets lack them. Many older adults face suboptimal intake of these essentials, fueling self-medication with supplements despite limited evidence.
Experts Caution Against Broad Claims
Cardiologists advocate a “food first, supplements last” approach, insisting lifestyle changes like DASH or Mediterranean diets outperform pills. Stanford Medicine experts reinforce that most well-nourished people gain no benefit from routine multivitamins and risk unnecessary costs or harms. Major guidelines do not recommend them for cardiovascular prevention in healthy populations.
Media headlines risk overstating subgroup signals as universal wins, potentially misleading consumers. Supplement makers may exploit the nuance for marketing, ignoring the null overall results from this robust trial.
Implications for Older Americans
For those with adequate diets, clinicians can dismiss multivitamins for blood pressure control. Poor-diet individuals with normal baseline pressure might see minor gains, but improving food choices yields greater rewards. This aligns with conservative values of personal responsibility in health, rejecting wasteful spending on unproven fixes amid inflation from prior fiscal mismanagement.
Future research could target deficient groups or specific nutrients. Guideline panels may note selective roles if replicated, prioritizing cost-effective nutrition over supplements. Public health should focus on food access for vulnerable seniors rather than diverting to pills.
Sources:
Daily multivitamins quietly lower blood pressure in some older adults
Vitamin B12, pills lower BP in old age? Cardiologist says ‘food first’
Long-Term Effect of Multivitamin Supplementation on Incident Self-Reported Hypertension and Blood Pressure in Older Adults: The COcoa Supplement and Multivitamin Outcomes Study (COSMOS)
Supplements: Five myths worth busting
Cocoa Extract and Incident Hypertension in the COSMOS Trial




























